- Membership Resources
- State Chapters
- Education/Events
-
Advocacy/Policy
- Home Care Workforce Crisis: An Industry Report and Call to Action
- Advocacy Fund
- State of Home Care: Industry at Crossroads
- Home Care Workforce Action Alliance
- Caring for Seniors: Value of Home Care
- Home Care by the Numbers
- Issues & Positions
- Legislative Action Network
- State Legislation Tracker
- Federal Legislation Tracker
- 2024 National Advocacy Day
- About HCAOA
- Find a Job
 CMS has addressed operational issues causing people to lose their Medicaid coverage during the federal unwinding period. CMS identified problems with how certain states auto-renew enrollees at the family level rather than the individual level, potentially leading to the improper disenrollment of eligible individuals when family members don't qualify for coverage. In response, CMS has mandated that affected states pause procedural terminations for those improperly disenrolled, reinstate their coverage, switch to individual-level auto-renewals, and implement strategies to mitigate further issues, such as extending Medicaid eligibility for affected families up to a year after their scheduled renewal period. CMS aims to rectify flaws in a renewal process that has resulted in millions of individuals losing Medicaid coverage because of the end of COVID-19 eligibility requirements.
0 Comments
 Representative Jesse Petrea has forwarded an update that he received earlier today concerning the approaching deadline of September 15th for all Medicaid providers to revalidate their credentials. This revalidation process must be completed to assure that providers continue to receive their Medicaid reimbursements for services rendered to Medicaid members.  Join Vicki Hoak, HCAOA’s CEO, on Thursday, September 21, 2023, at 12:00 p.m. ET for a webinar discussing trends in home care mergers and acquisitions. She will be joined by colleagues from Polsinelli and the National Association for Home Care & Hospice. During this webinar, attendees will hear from active buyers who will share their experiences in home care agency acquisition transactions and discuss their criteria when targeting agencies for acquisition. The webinar will also cover the mechanics of a home-based care transaction, covering various transaction types and options, the legal framework of a deal, regulatory considerations, pitfalls in the diligence process, and essential steps agency owners should take to prepare their agency for sale. The aging U.S. population is expected to increase the demand for long-term services and supports (LTSS), much of which is currently provided by informal caregivers. However, for those requiring paid LTSS, most Americans rely on personal funds and then turn to Medicaid once their resources are depleted. This reliance on Medicaid for individuals with limited income and assets could increase federal and state spending on LTSS. To address this concern, a project was initiated to analyze the current cost of long-term care, national expenditures on LTSS, and future predictions regarding the availability of informal caregivers. The project explores how demographic changes will impact the supply of informal caregivers for older Americans. One of the project's primary goals is to provide updated estimates of national LTSS expenditures and projections that illustrate how changing demographics may affect the demand for LTSS, the availability of future caregivers, and Medicaid spending.
 Krystal Wilkinson, HCAOA Arizona Chapter Chair and President of Adultcare Assistance (second from right), and Stephanie Roberts, Policy Leader with Team Services Group (left), recently met with two Arizona state representatives, Rep. Patty Contreras (D-12) and Rep. Judy Schwiebert (D-2), to discuss home-based care issues, including Medicaid reimbursement rates and how to ensure safety in home care in Arizona.  An article entitled, “Price of elder care soars as demand increases, baby boomers age,” was published on TheHill.com on August 13, 2023. The article discusses how the cost of caring for aging or ailing family members in the U.S. has risen dramatically in recent years in nursing homes, assisted living facilities, and adult day centers. With insufficient support from programs like Medicare and Medicaid, many family caregivers are forced to deplete their limited funds to cover expenses. Alaska recently passed legislation (SB.57) to expand home care access for aging adults and others requiring assistance with daily living through a new Medicaid service called "adult home care,” expected to affect 2,500 residents. Signed into law on July 29 as part of the governor's Healthy Families Initiative, the option will enable more individuals to receive medical and personal care at home rather than having to move into costlier institutional settings like nursing homes. The law is part of Alaska's efforts to improve health equity and meet the needs of older adults within their communities.
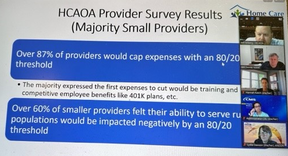
HCAOA continues efforts to highlight the negative impact of CMS’ proposed rule that would require states to ensure at least 80 percent of all Medicaid HCBS payments are spent on compensation for direct care workers, such as nurses, home health aides, and others who directly support Medicaid beneficiaries in activities of daily living at home. The remaining 20 percent of payments would be expected to cover all other HCBS operating expenses.
 HCAOA New York Chapter Co-chair and owner of Right at Home – North Shore Long Island Zubin Kapadia met recently with New York State Senator Joseph P. Addabbo, Jr. (D-15) to discuss critical legislative matters. Sen. Addabbo said he supported the legislation to increase caregiver wages in the 2022 budget, which Kapadia also supports, and recognizes the need to incentivize and retain good aides. However, he noted that the legislation was driven principally by the proponents of labor, and thus the impact on private pay agencies and seniors was not fully considered. Zubin Kapadia stated, “I laid the blame for that on us as business owners to do more to educate the legislature on the downstream impact of these laws; i.e. private pay client rates will increase, families will be burdened with paying more out of pocket, and many will file for state Medicaid or go to the gray market for care. I noted that most of our clients are “family funded” and there is a huge misconception that private pay homecare is only for the wealthy. I mentioned that as opposed to Medicaid agencies, we will not get any offset in the form of higher reimbursements, and thus a tax credit would be the most appropriate way to protect seniors and level the playing field.” In 2019, a review conducted by the Office of Inspector General (OIG) found that Managed Care Organizations (MCOs) denied approximately one out of every eight requests for prior authorization of healthcare services. The study examined 115 MCOs and discovered that 12 of them had prior authorization denial rates exceeding 25%, double the overall rate. The American Association for Homecare (AAHomecare) summarized the OIG report, which highlighted the lack of mechanisms for patients and providers to challenge MCO denials, and recommended that the CMS take several actions to improve oversight, including regular reviews of MCO prior authorization denials, data collection, issuing guidance to states, implementing external medical reviews, and addressing inappropriate denials.
 Last week, HCAOA Board President Jeff Wiberg and CEO Vicki Hoak met with CMS Administrator Chiquita Brooks-LaSure to discuss the Medicaid Proposed Rule, which would require 80% of Medicaid reimbursement to go to worker wages. HCAOA was one of four national groups in the meeting, including the American Network of Community Options and Resources (ANCOR), the National Association for Home Care and Hospice (NAHC), and the Partnership for Medicaid Home-Based Care (PMHC). After coordinating with a broad cross section of members and recognizing the strength in collaboration, HCAOA teamed up with the National Association for Home Care & Hospice (NAHC) to develop and submit formal comments to CMS on the Medicaid HCBS proposed rule released in May. Both associations are supportive of many of the provisions in the proposed rulemaking, however did offer suggestions to improve several provisions.
Effective July 1, 2023, the Connecticut Department of Social Services, in response to the increase in the minimum wage, is increasing rates by 4.9% for several Home and Community Based waiver service providers, the Department announced in a policy bulletin on June 30. The programs include the Connecticut Home Care Program for Elders and Personal Care Assistance.
Effective July 1, 2023, the South Carolina Department of Health and Human Services (SCDHHS) is consolidating multiple personal care and private duty nursing services into single procedure codes for personal care, private duty nursing and enhanced nursing. These service consolidations are being made to reduce the administrative burden for providers and support improved access to care. These changes affect State Plan private duty nursing services and services provided through home and community-based service (HCBS) waiver programs.
|
Archives
April 2024
Categories
All
Upcoming Events |
|
Phone: 202-519-2960 | 444 N. Capitol Street NW, Suite 428 | Washington, DC 20001
info@hcaoa.org | sitemap © 2024 Home Care Association of America. All Rights Reserved. | Privacy Policy | Refund Policy |
|


 RSS Feed
RSS Feed
